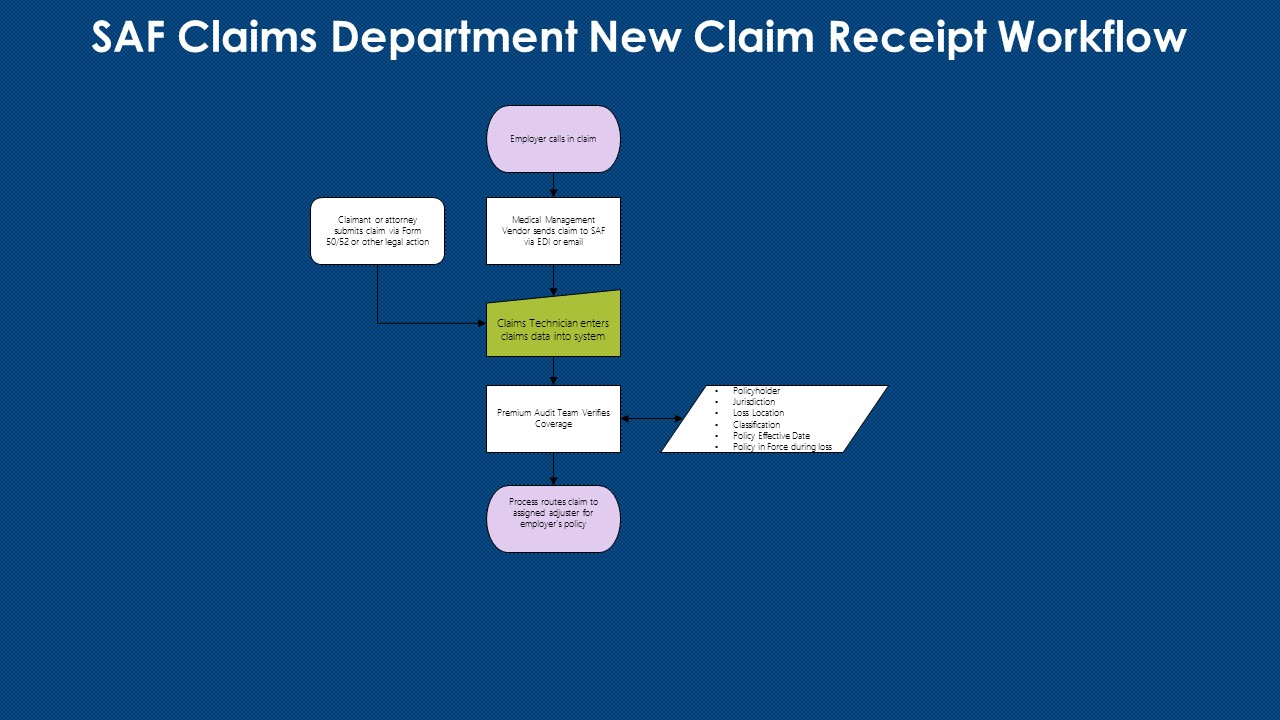
Report an Injury
It is the responsibility of the employee to report an injury, as soon as possible, to their employer (supervisor, human resources, etc). The employer will then report the claim to the appropriate Medical Management Vendor, who will assign a nurse case manager to direct all medical care for the injured employee. The nurse case manager also provides treatment authorization, as well as appropriate billing information to the medical provider. All pertinent information will be relayed to the assigned adjuster at the State Accident Fund.
Once the claim has been assigned to an adjuster, all information will be reviewed to determine claim compensability (claim acceptance or denial). The adjuster may need to contact the injured employee prior to this determination if any additional information is required. The injured employee will receive a letter in the mail from the State Accident Fund regarding this compensability decision. The assigned adjuster’s contact information will be included in this letter, as well as a mileage reimbursement form and a medical release form.
If the claim is accepted, all medical treatment will be directed by the adjuster and nurse case manager. The nurse case manager will handle the scheduling of all treatment, appointments, etc. It is the responsibility of the injured employee to comply with the treatment arranged by the nurse case manager.
The State Accident Fund reserves the right to deny treatment if an injured employee elects to seek treatment on their own, or is non-compliant with the treatment arranged by the nurse case manager or adjuster. If an injured employee has any questions or concerns regarding their treatment and/or schedule, it is their responsibility to contact their nurse case manager or adjuster as soon as possible.
If you have questions regarding your claim or need to contact your nurse and adjuster please e-mail claims@saf.sc.gov and reference your full name and claim number or call us at 803-896-5800.
If you wish to file a claim directly with the South Carolina Workers' Compensation Commission, you can do so by using Form_50 (PDF) or by visiting The SC Workers' Compensation Commission forms page.